Why this article exists
A meaningful share of the work that walks through our doors is work someone else started. Patients arrive with veneers, crowns, bridges, or full reconstructions that didn't end where they hoped — sometimes within months of placement, sometimes years later. Some are referred by other dentists who recognized the case had grown beyond their scope. Others come on their own, having lived with restorations they were never quite happy with.
We see enough of it that we've built our practice around doing it well. This article is for the patient sitting on the other side of that experience: living with dental work that doesn't look right, doesn't feel right, or doesn't fit right, and trying to figure out whether it's worth doing something about it.
What 'redoing' actually covers
When patients come to us for a redo, the original concern almost always falls into one of four categories. Often it's more than one at once.
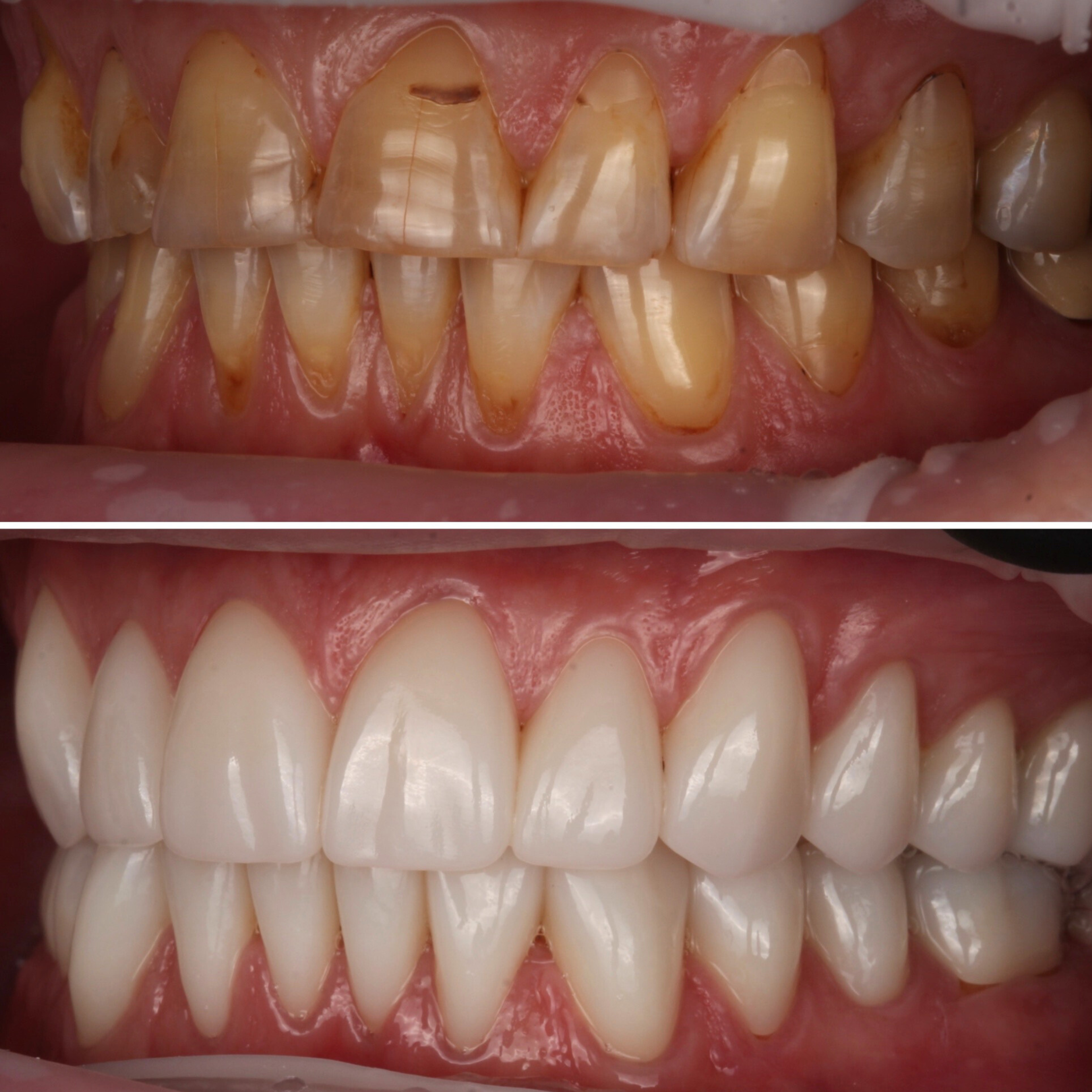
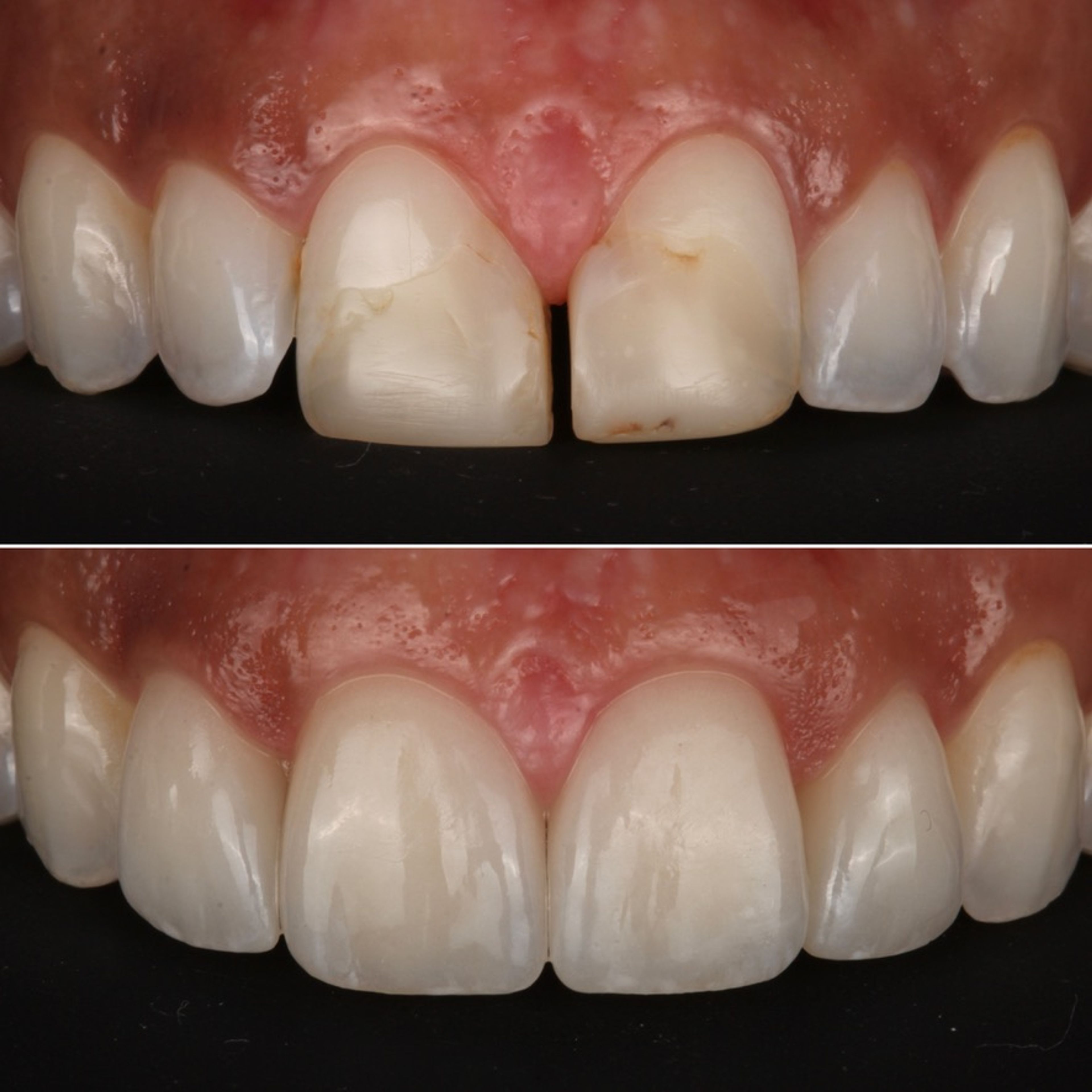
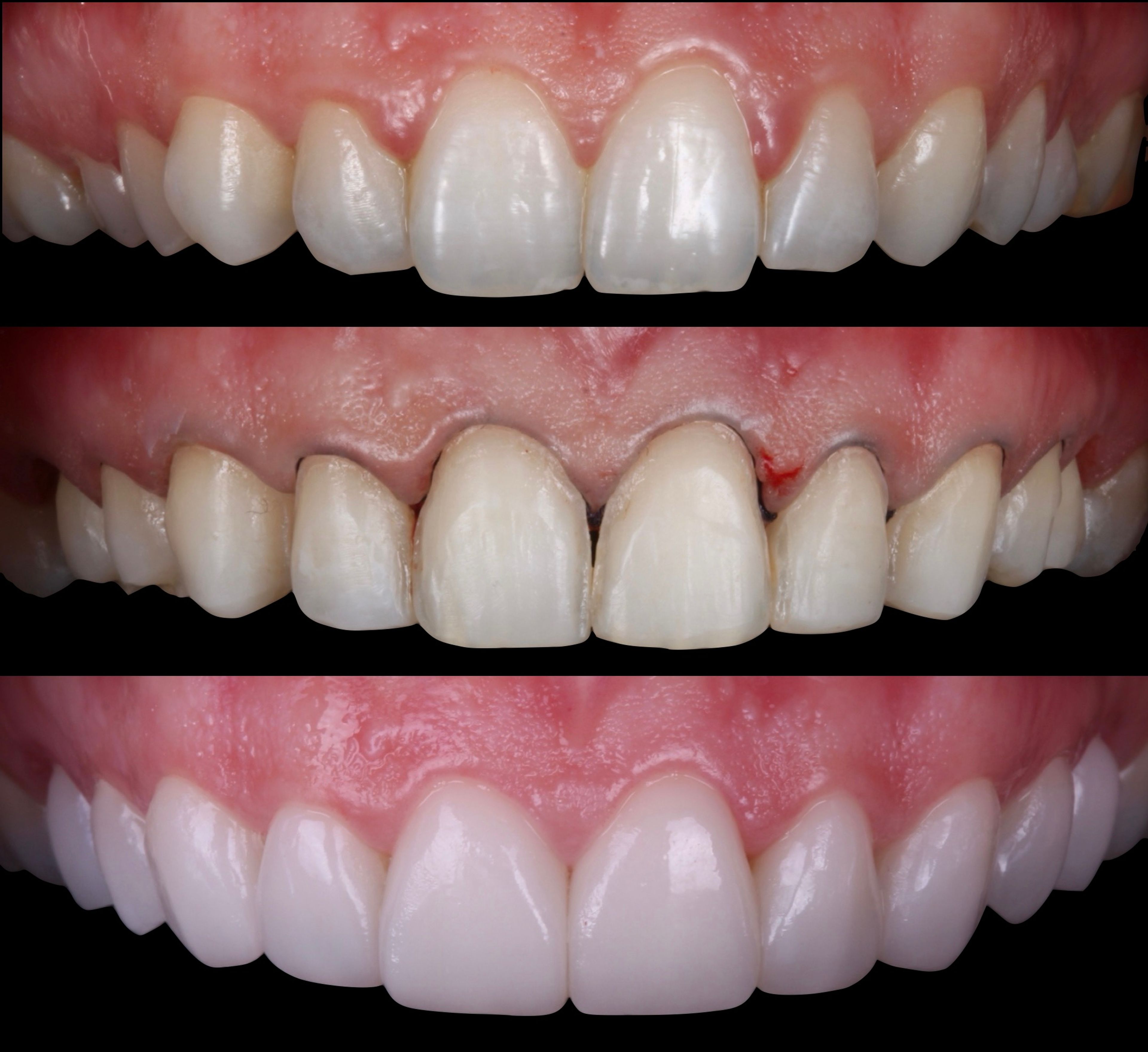
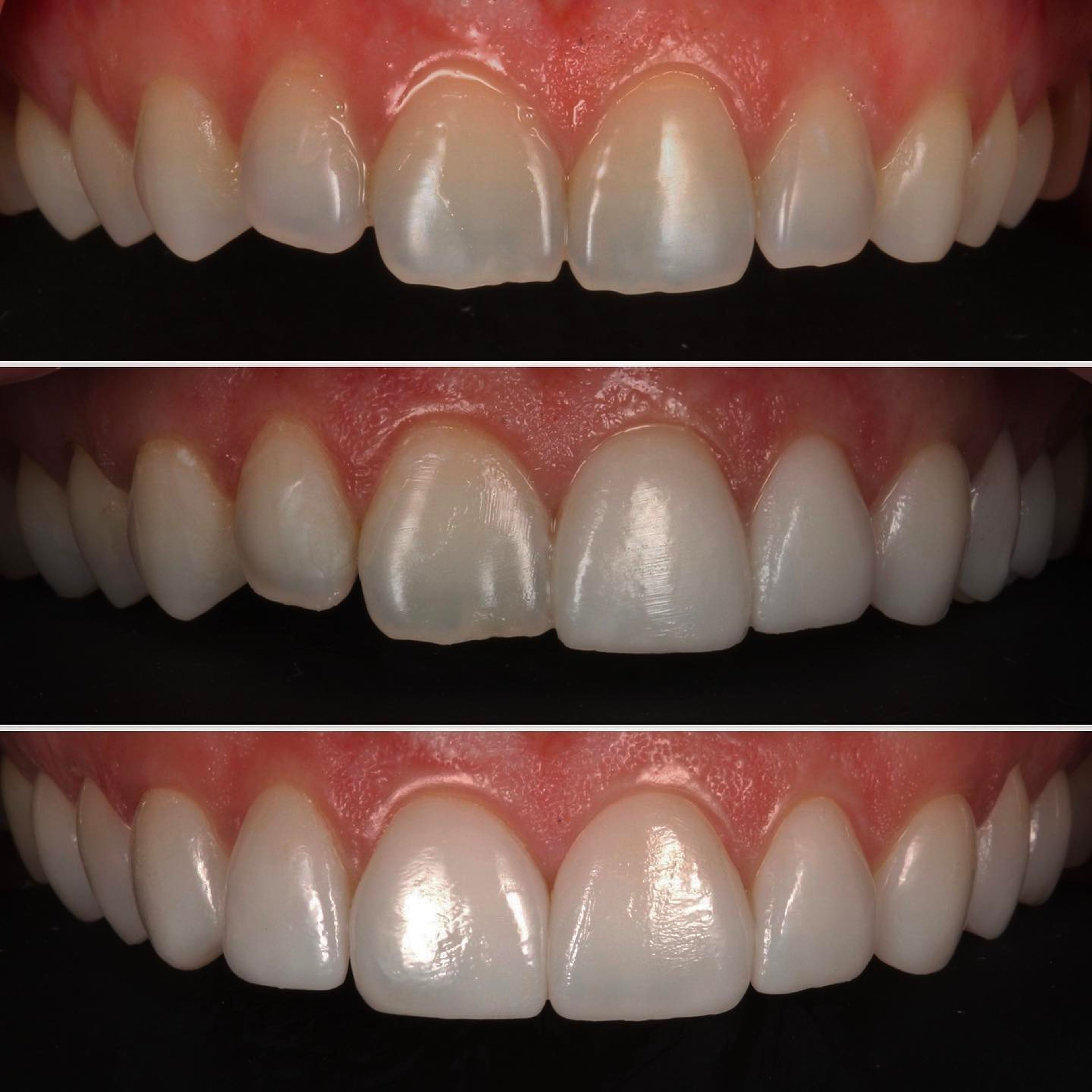
Aesthetics. The most common reason. Sometimes the restorations look too uniform — every tooth the same shade, the same shape, the same translucency, in a way no natural smile ever is. Sometimes margins are visible where the porcelain meets the tooth. Sometimes the result looks too natural — the patient wanted a more significant change to their smile and didn't get it. The common thread: the smile doesn't feel like the patient's own, in either direction.
Bite and function. Especially in larger reconstructions, the way the teeth meet matters as much as how they look. A bite that's even slightly off can cause discomfort when chewing, jaw fatigue, sensitivity, or chronic tension that the patient may not initially connect to their dental work. Getting the bite right in a complex case is a separate craft from getting the aesthetics right, and not every restoration that looks good actually functions well.
Fit. Restorations are supposed to seat against the tooth seamlessly. When they don't — when there's a gap between the edge of the porcelain and the tooth underneath — the consequences compound. Plaque collects in the gap. Bacteria settle in. Cavities can form underneath the restoration, often invisibly, until they've gotten serious.
Tissue health. Closely related to fit. When restorations don't adapt well to the tooth at the gum line, the gums respond with chronic, low-grade inflammation. Patients describe it as gums that bleed when brushing, persistent bad breath that doesn't respond to better hygiene, or just a vague sense that something around those teeth is wrong. The tissue knows when a restoration doesn't fit.
And here's the diplomatic truth that experienced clinicians know: more often than not, when a restoration fails on any of these dimensions, it isn't because the dentist made a clinical error. It's because the lab the work was sent to didn't deliver — the porcelain wasn't shaped quite right, the shade wasn't matched, the margins weren't crafted to seat the way they should. The dentist did their part; the lab let the case down. Working with a lab team you trust, in close collaboration, is what prevents this. It's also why so many redos route to practices with their own in-house labs.
What 'fit' really means
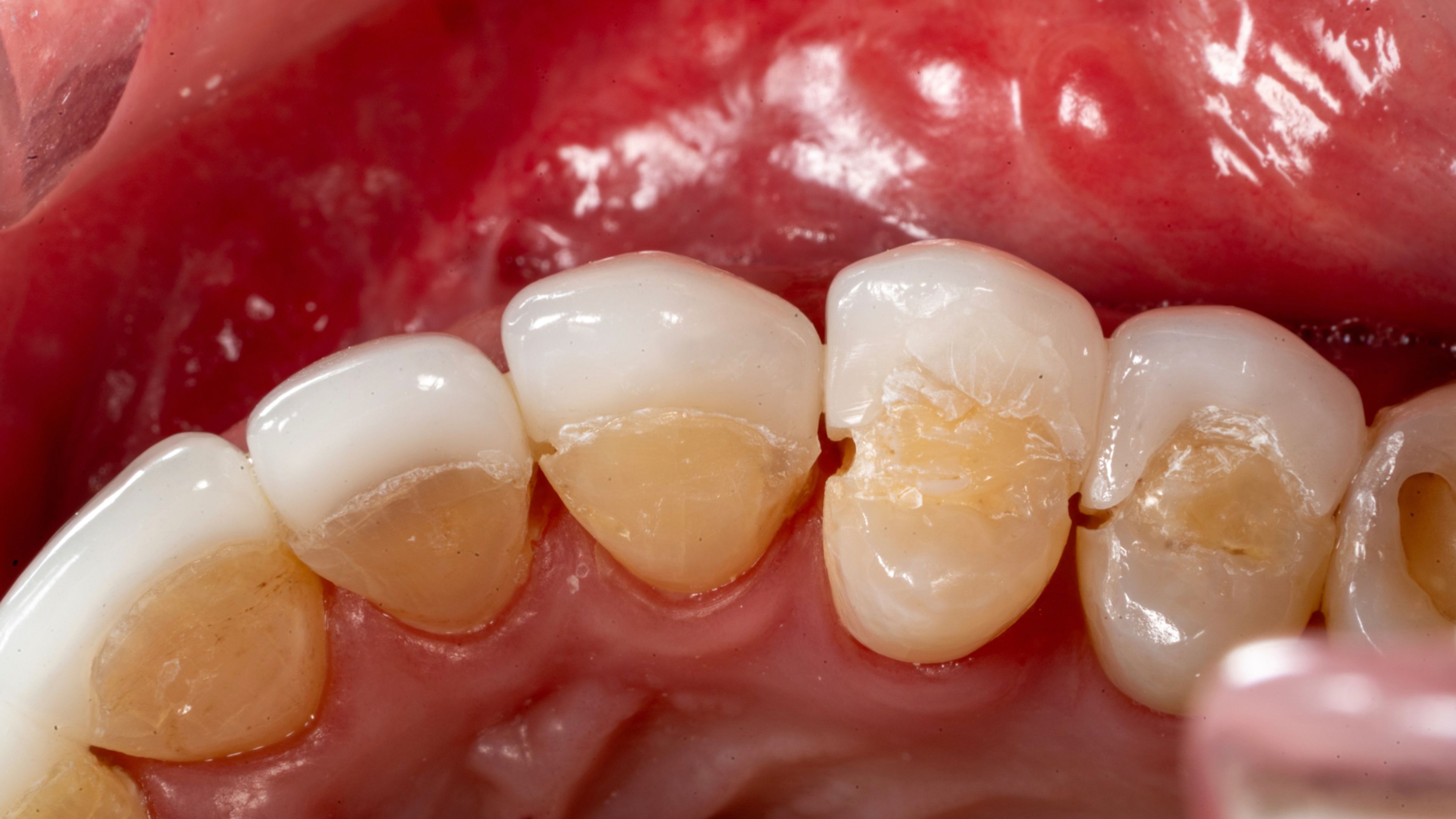
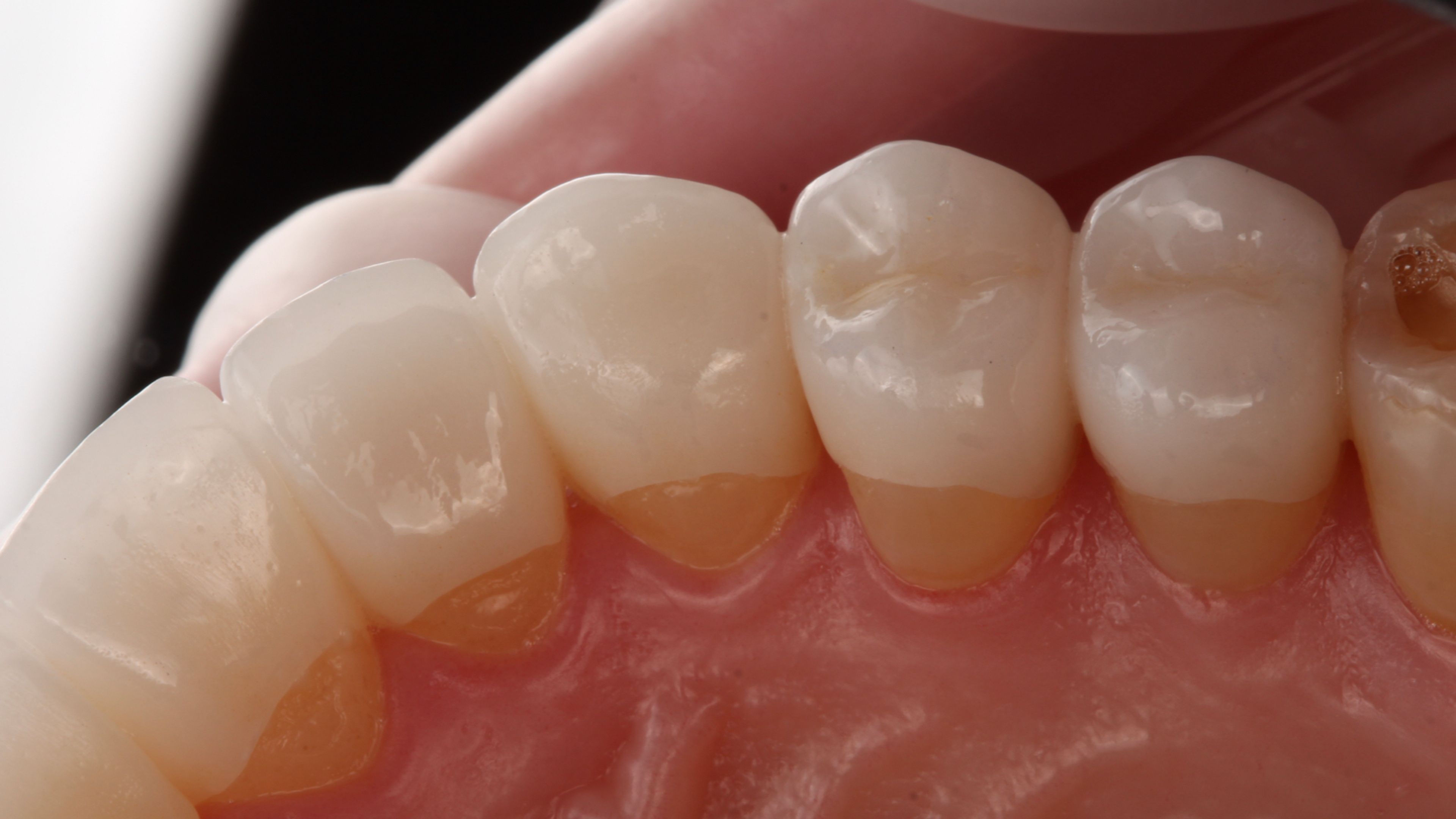
When it's worth redoing — and when it isn't
Not every restoration that bothers a patient needs to be replaced. Part of an honest consultation is sorting out which complaints justify the time, cost, and biological investment of a redo, and which are better lived with.
Reasons we usually recommend redoing the work:
- The fit is poor enough that it's putting the underlying tooth or the surrounding gums at risk.
- Chronic gum inflammation around the restoration that won't resolve with hygiene improvements — the tissue is telling us something.
- Aesthetic concerns the patient genuinely cannot live with. We don't try to talk anyone into accepting a smile they don't recognize as their own.
- Bite issues causing pain, sensitivity, or muscle tension — these tend to get worse, not better, the longer they go unaddressed.
- A restoration that has cracked, chipped, or otherwise mechanically failed.
Reasons we sometimes recommend leaving the work alone:
- The aesthetic concern is minor and a redo would carry more risk to the underlying tooth than benefit to the smile.
- The restoration is functioning well, the tissue is healthy, and the patient is undecided.
- The patient hasn't given the original work enough time to settle — sometimes what feels wrong in the first weeks normalizes as the bite and tissue adapt.
The conversation isn't about selling a redo. It's about diagnosing what's actually happening and giving the patient a clear-eyed read on whether change is justified.
The hidden problem with how restorations are usually removed
If a redo does make sense, the way the original work comes off matters more than most patients realize.
The conventional approach to removing a porcelain veneer or crown is to cut through it with a high-speed bur — essentially grinding the porcelain off in pieces until the underlying tooth is exposed. The problem isn't that this can't be done; the problem is that it generates significant heat, and the bur can't always tell where the porcelain ends and the tooth begins. By the time the restoration is off, the tooth underneath has often been thinned further, sometimes meaningfully. Heat can also irritate the nerve and lead to sensitivity that takes weeks to resolve, or in worse cases, doesn't resolve at all.
On a tooth that's already been prepared once for a restoration, every additional fraction of structure removed matters. The tooth started its restorative life with less than full thickness. Conventional removal subtracts more. After a redo done this way, the tooth is in a worse position than when the original work was placed.
There's a better way.
Removing porcelain with an erbium laser
We removed enough restorations over the years that we eventually invested in a piece of equipment most general practices don't have: an erbium laser specifically suited to atraumatic porcelain removal. It's expensive, the technique takes training, and the patients we see for redos are the reason it's worth it.
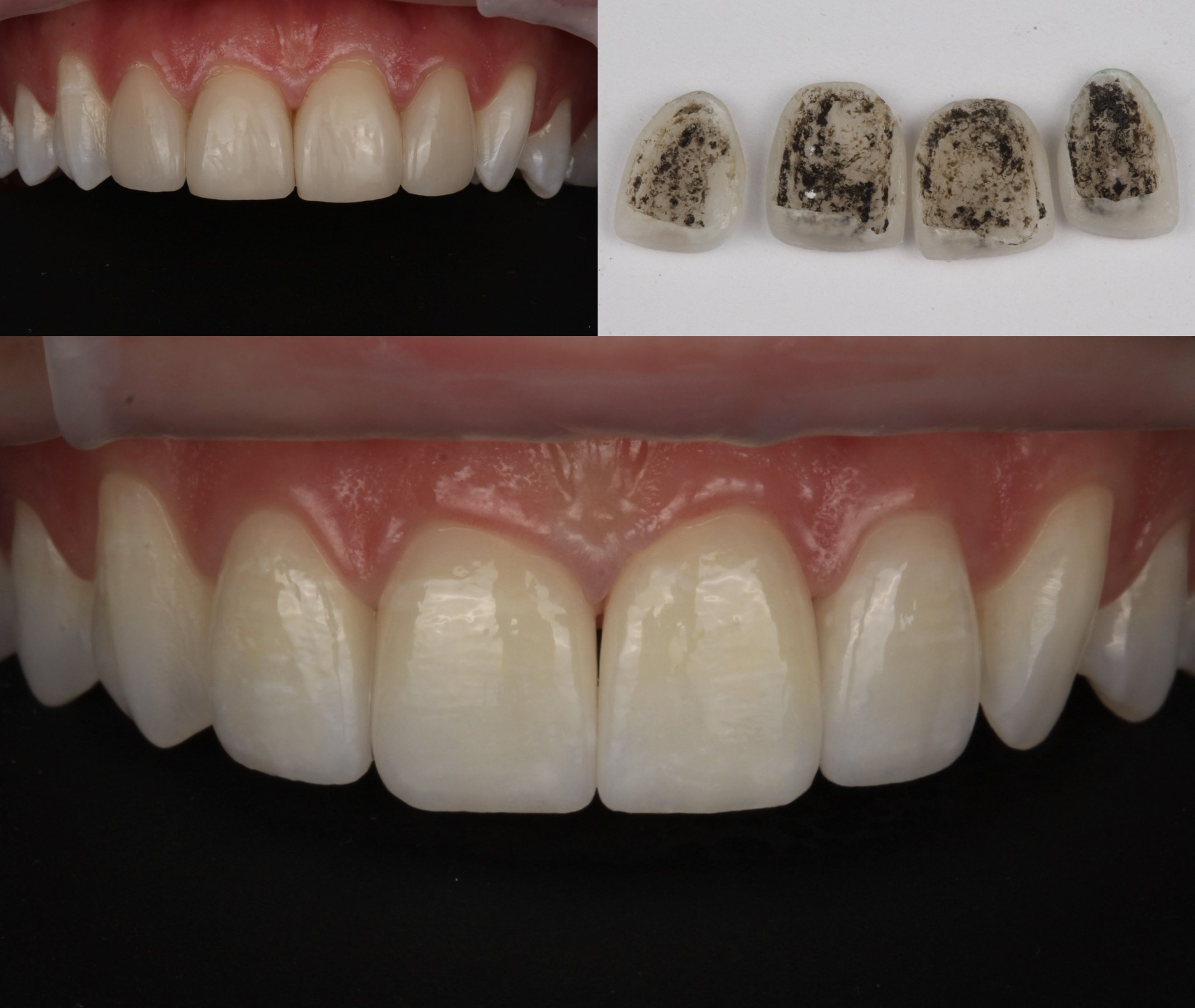
What the laser does that a bur cannot: it targets the bonding interface between the porcelain and the tooth. The laser energy passes through the porcelain and heats the bonding layer just enough to break its hold on the enamel underneath. The restoration releases — often in a single piece — without the porcelain ever being cut through, and without the tooth being touched by anything mechanical.
What this means in practice:
- The original tooth structure is preserved. We remove the restoration, not the tooth.
- There's no heat damage to the underlying tooth or pulp. The energy is absorbed at the bonding layer and dissipates harmlessly.
- Postoperative sensitivity is dramatically lower than after conventional removal. Many patients feel essentially normal the next day.
- We learn things about the original case we couldn't have learned otherwise. Once the porcelain comes off cleanly, we can see exactly what the original prep looked like — and sometimes that information changes the entire treatment plan.
That last point is worth its own section, because it's the most surprising thing about doing redos this way.
A case that became something different than we expected
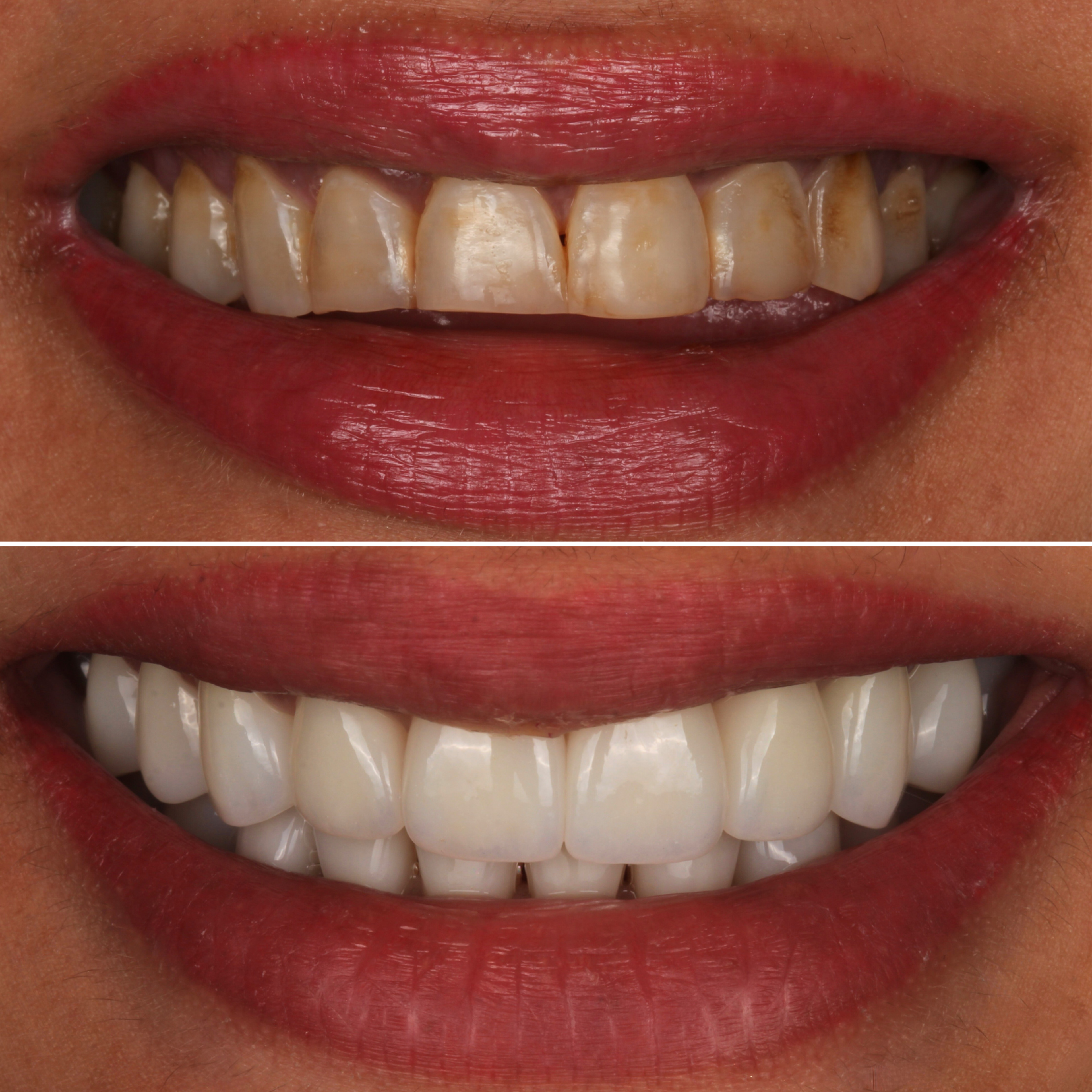
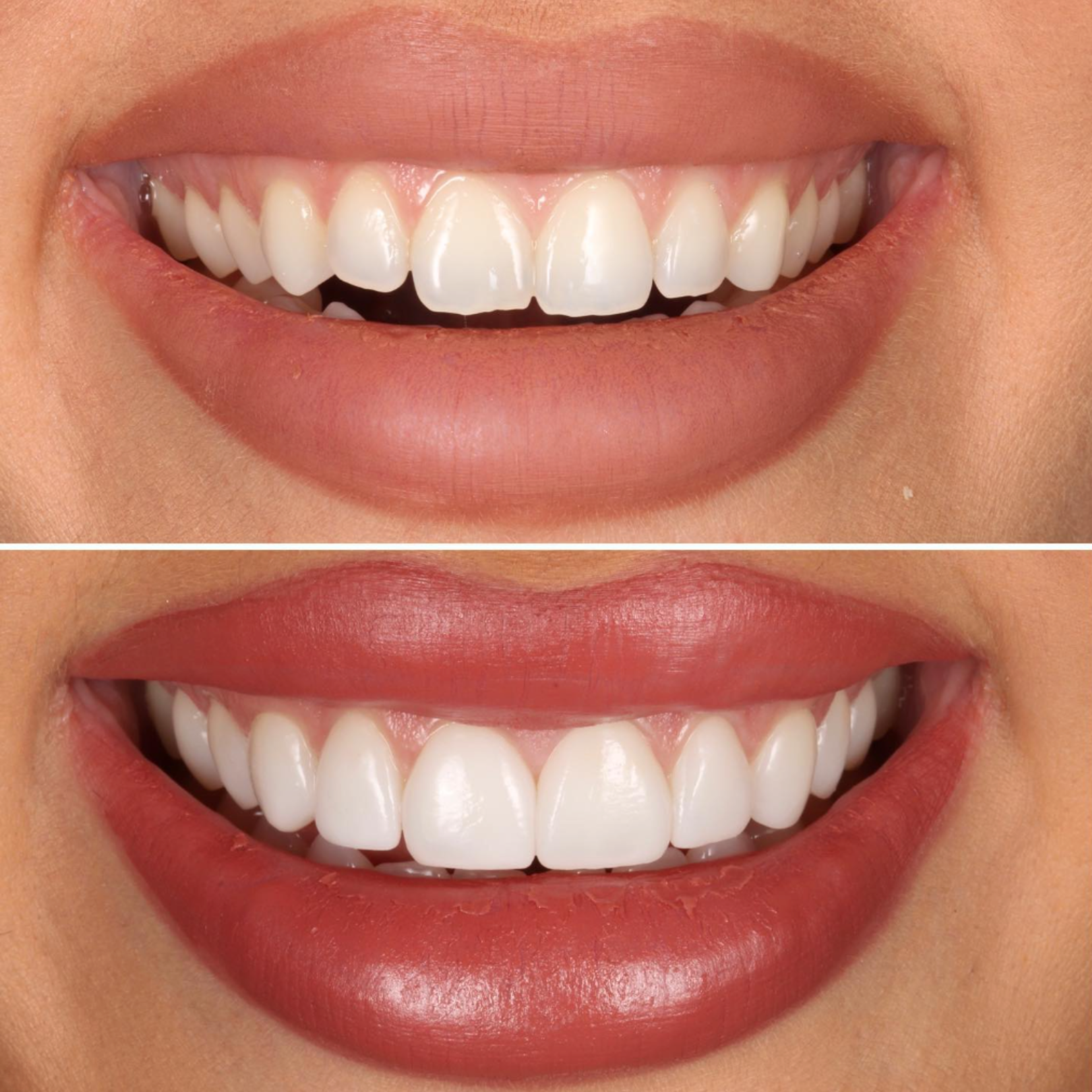
A patient came to us a few months after having twenty porcelain veneers placed elsewhere — ten on top, ten on the bottom. He hated them. He told us he wished he could go back to his original smile and that he regretted the whole thing.
Twenty veneers becomes four
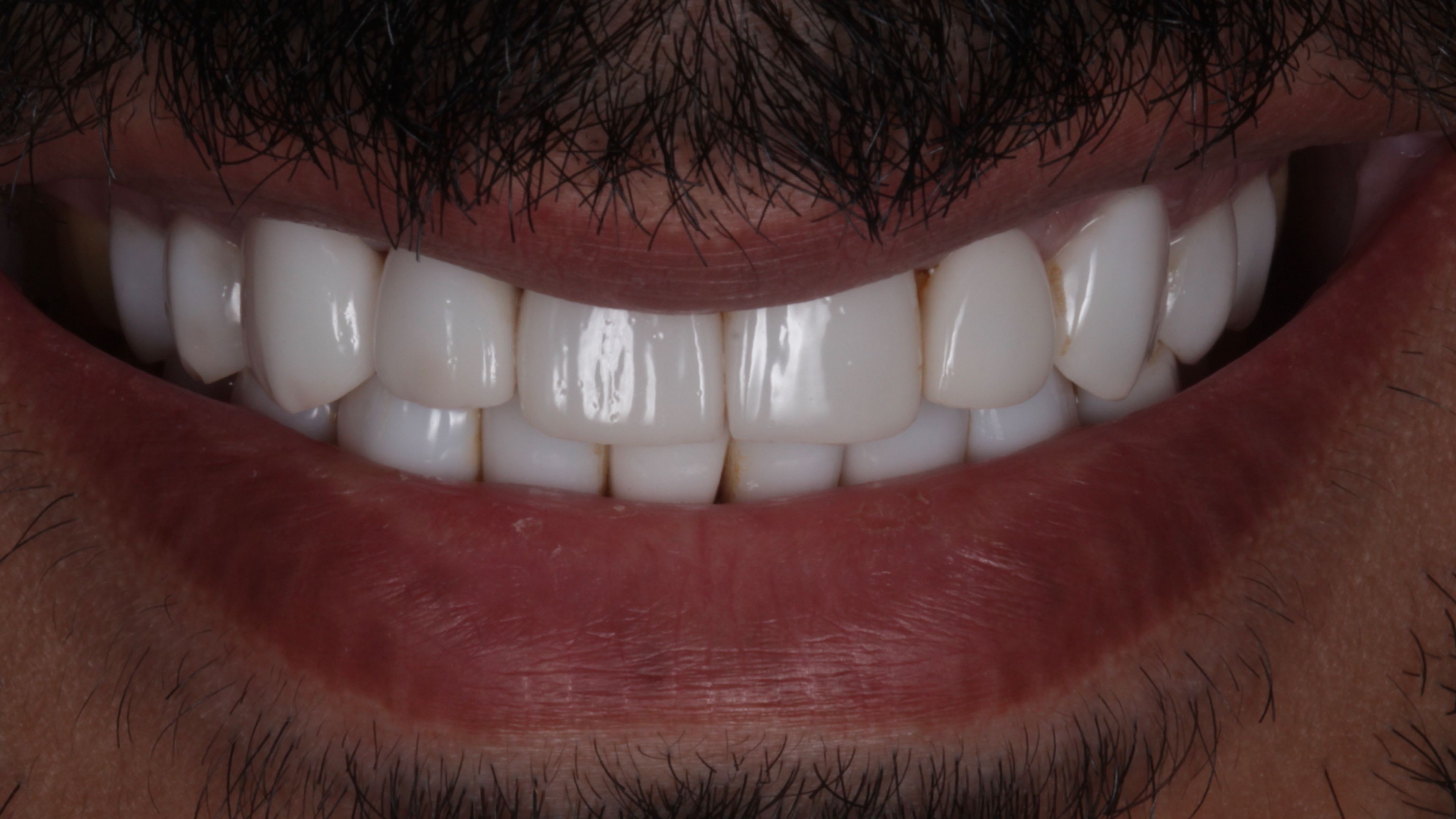
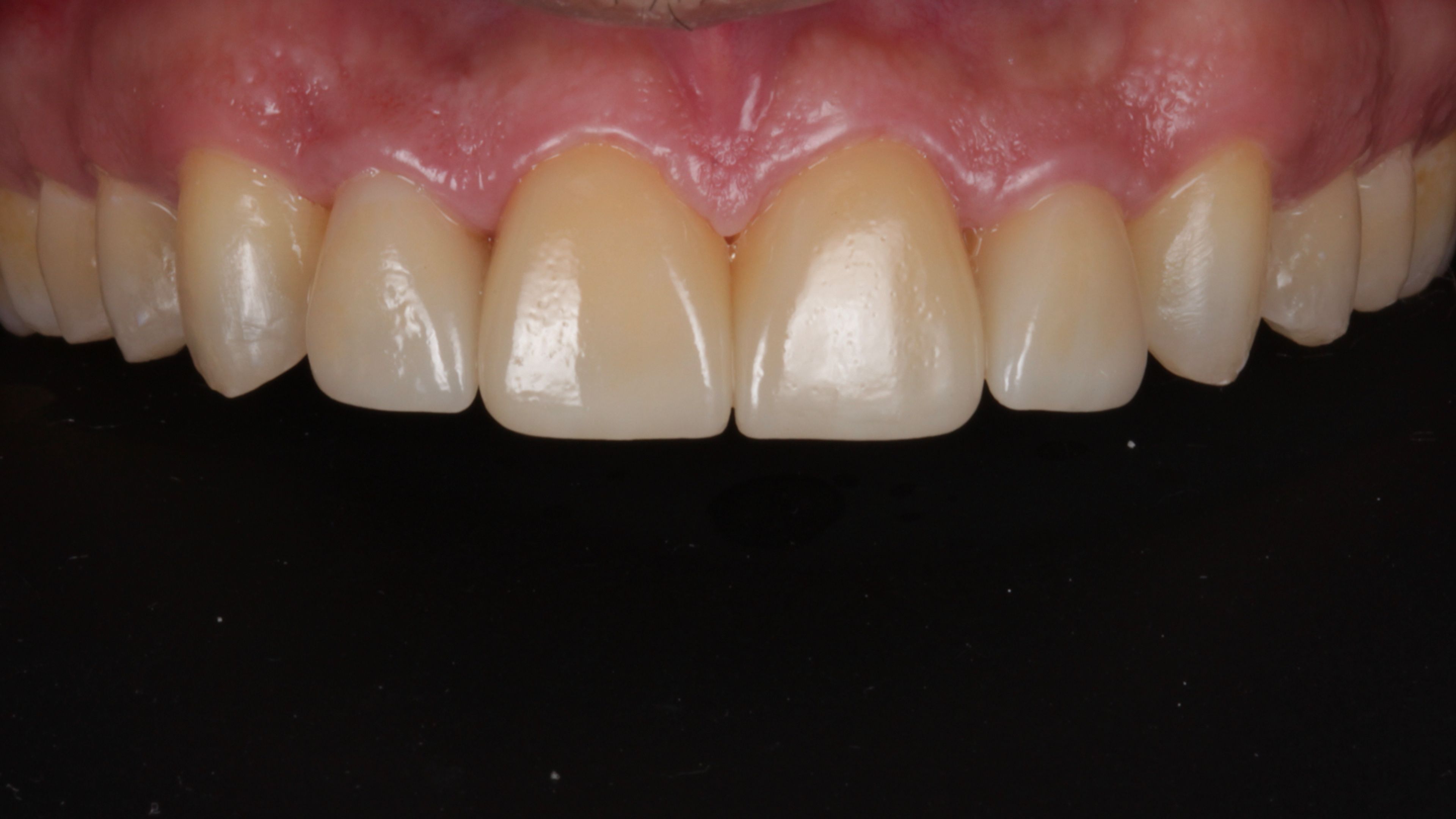
Normally, once a patient has had veneers, the option to go back to the original teeth is off the table. Even minimal preparation removes some structure, and the way porcelain bonds to that prepared surface means the only practical replacement for a veneer is another veneer. Our plan, going in, was to redo all twenty in a more natural-looking design.
But because the laser removed the original veneers without touching the teeth underneath, we got a clean look at what had actually been done to his teeth in the original case. The preparation, it turned out, was minimal — almost none in places. Most of his teeth were essentially intact. That gave us an option we couldn't have anticipated: rather than replacing all twenty veneers, we could keep the vast majority of his teeth as his own natural enamel, and place only four new veneers on the front to address the spacing concern that had brought him to veneers in the first place.
The same case, up close
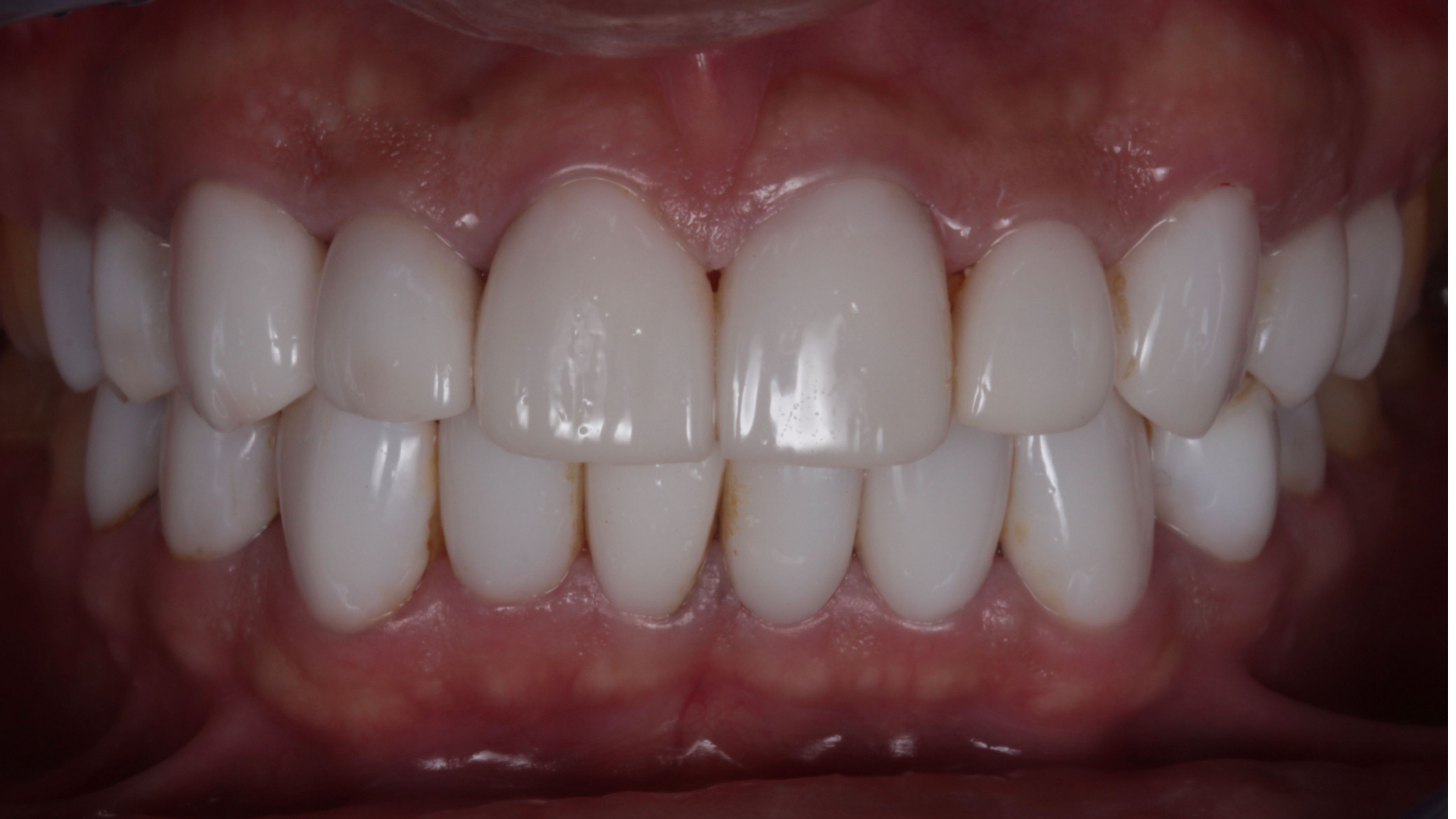
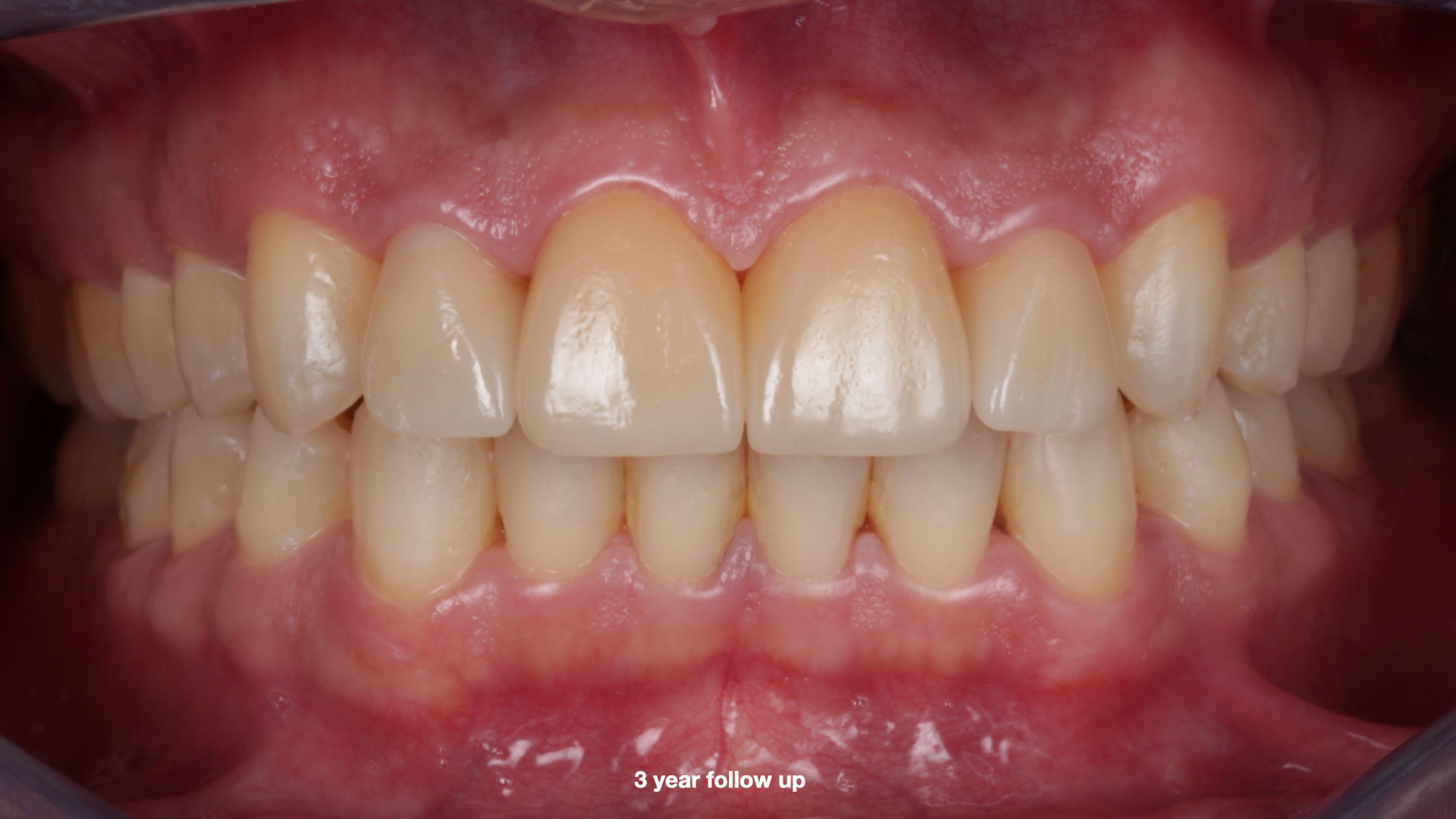
He went from twenty veneers to four. Most of his smile is his own teeth. This outcome is rare — most redo cases come to us with more aggressive original preparation, and the only path forward is replacement with new restorations. But it's an example of what becomes possible when you remove without damaging, and when you treat removal itself as a diagnostic step rather than a destructive one.
Why an in-house lab matters in redos specifically
Most cosmetic dentistry is a partnership between a dentist and a lab. The dentist prepares the tooth, takes records, and communicates the design intent; the lab fabricates the actual porcelain. When the partnership works, the result is beautiful. When it doesn't — when the dentist's intent and the lab's execution drift apart — the result is a redo.
If most redos trace back to lab-side issues, then the way to prevent the second case from going wrong is to bring the lab into the diagnostic process. That's a lot harder when the lab is in another city and communication happens through forms and shipping schedules.
Our ceramists and lab team work in the same building as our prosthodontists. When a redo case comes in, the lab team is part of the conversation from the first appointment. They look at the original restorations alongside us. They study the photographs. They evaluate what went wrong and what the new design needs to do differently. By the time we get to fabrication, the craftspeople making the new porcelain already know the patient, the case history, and the specific aesthetic and functional targets we're aiming for.
When something needs to be adjusted between try-in and final — a shade tweak, a contour refinement, a half-millimeter change to the length — it happens that day. Not next week, not after another shipment. The iteration loop is short enough that we can get the result exactly right rather than settling for close enough.
Redos demand iteration. The patient already has a sense of what they don't want, and getting from there to what they do want requires more refinement, not less.
The redo process, step by step
Diagnosis and treatment planning.
We start by figuring out what actually went wrong with the original work. Photos, examination, often a digital scan, and a careful conversation about what the patient experiences day to day — aesthetically, functionally, and in terms of comfort. The goal is to understand the failure modes specifically enough that the new plan addresses every one of them. A redo that doesn't begin with diagnosis is just a second roll of the dice.
Design phase with the lab.
We bring the new design to our lab team early. Together we map out shade, shape, length, and proportions, while also accounting for how the new restorations need to function — how they'll meet the opposing teeth, how the bite distributes, how the case ages. Aesthetics and function are designed in parallel, not one after the other.
Atraumatic removal.
Under local anesthetic, the original restorations are removed with the erbium laser. The underlying teeth are evaluated immediately afterward — sometimes the picture changes here, as it did in the case above.
Refinement (when needed).
If the original preparation was uneven or compromised, we refine the surfaces gently to give the new restorations a clean foundation. Often this is minimal. Sometimes it isn't needed at all.
Temporaries and fabrication.
The patient leaves the same day with provisional restorations approximating the new design. The temporary phase is a real test drive — patients evaluate how the new shape feels, how it looks in different lighting, how the bite functions during everyday life — and give us specific feedback. While that's happening, our ceramists craft the final porcelain in our in-house lab, working in close collaboration with the prosthodontist on every detail of shade, translucency, shape, and margin. Iteration is fast because the lab is steps away.
Try-in.
When the porcelain is ready, we try it in before any final insertion. The patient sees the new restorations in place, sits with them, and has the chance to ask for any final adjustment. Things can still change at this stage.
Final insertion.
When everything is right, the new restorations are inserted using modern adhesive protocols. Margins are polished so they're seamless to the eye and to the tongue. The patient walks out with the smile they came looking for.
A redo, start to finish
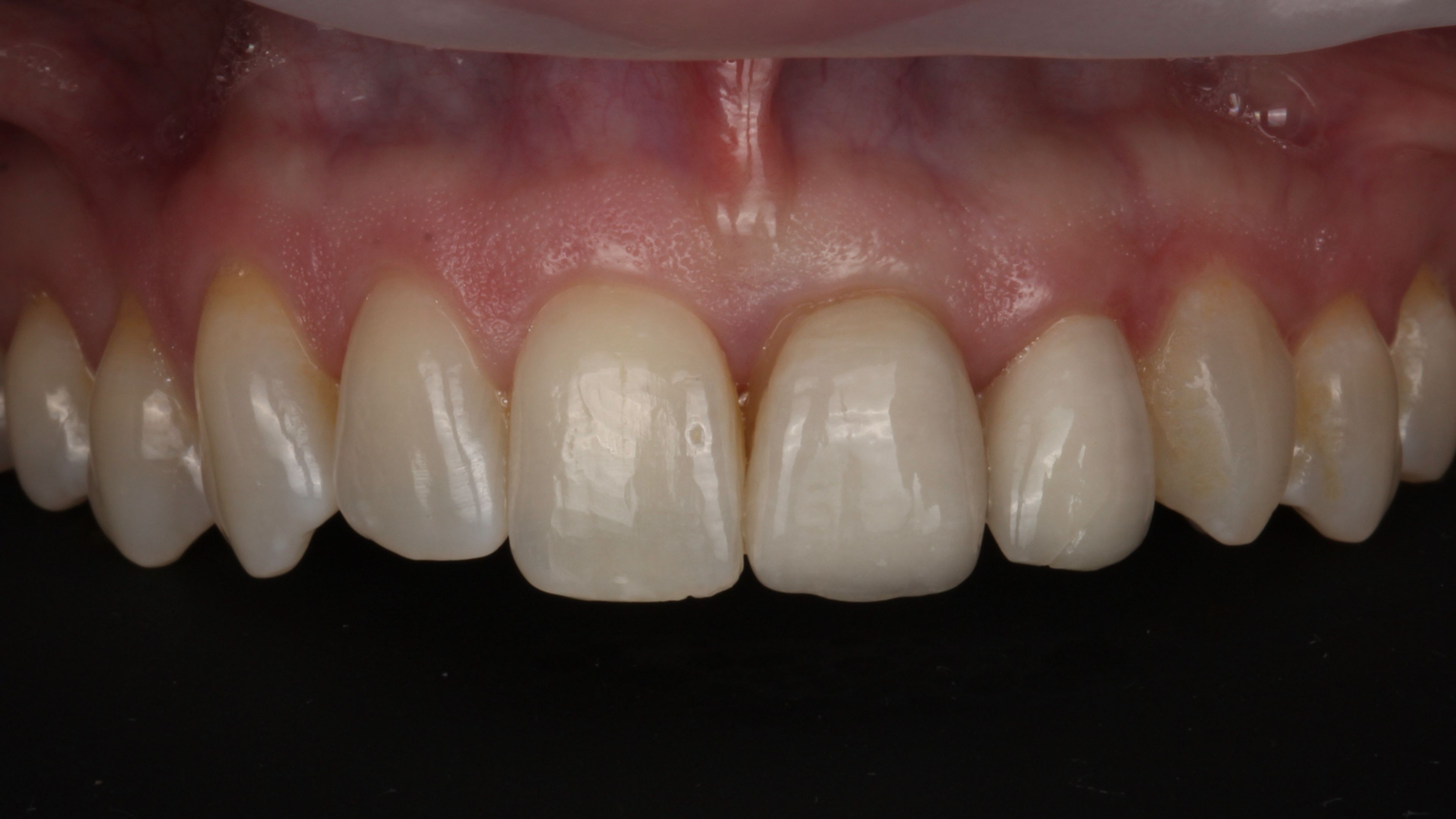
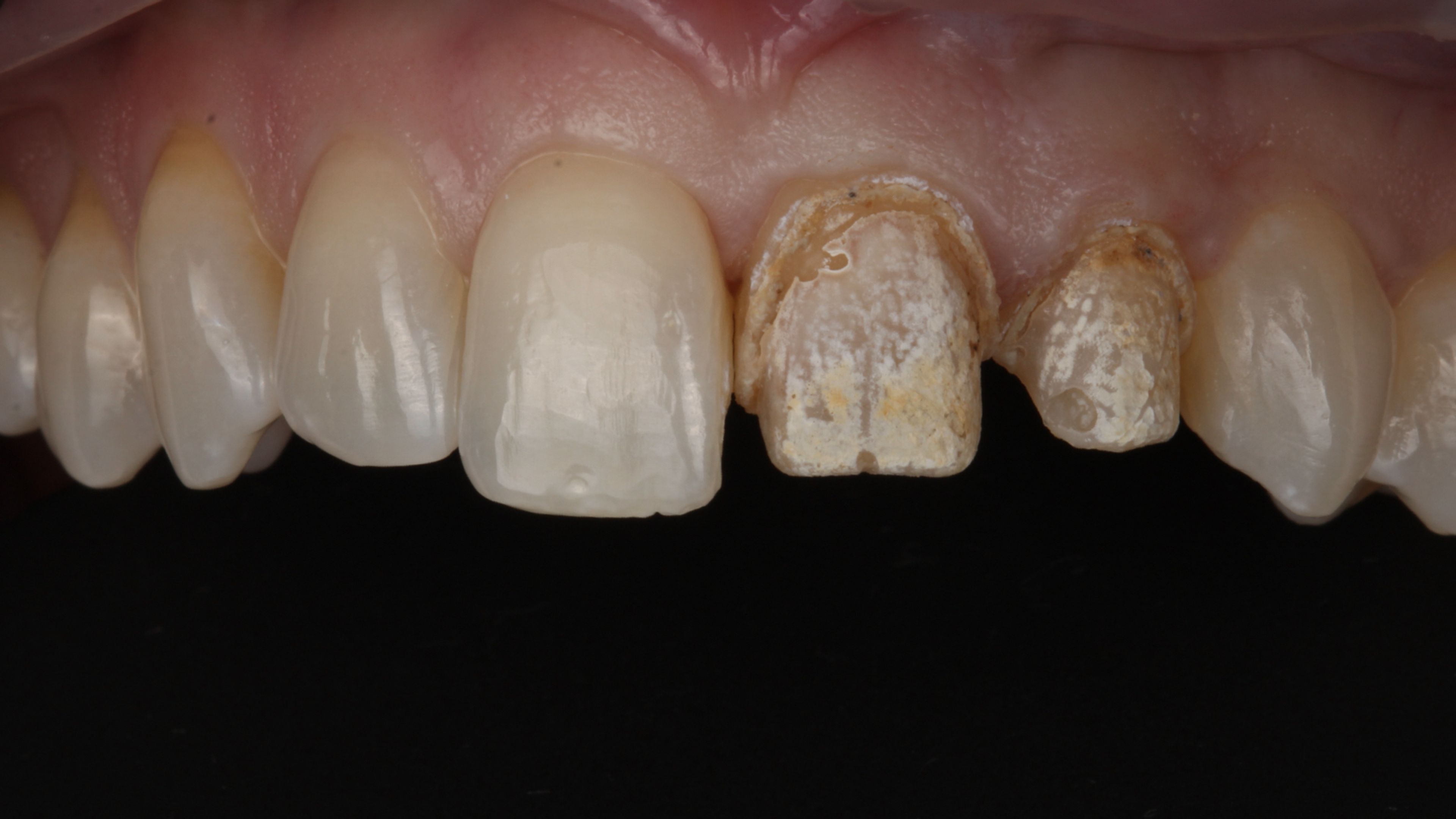
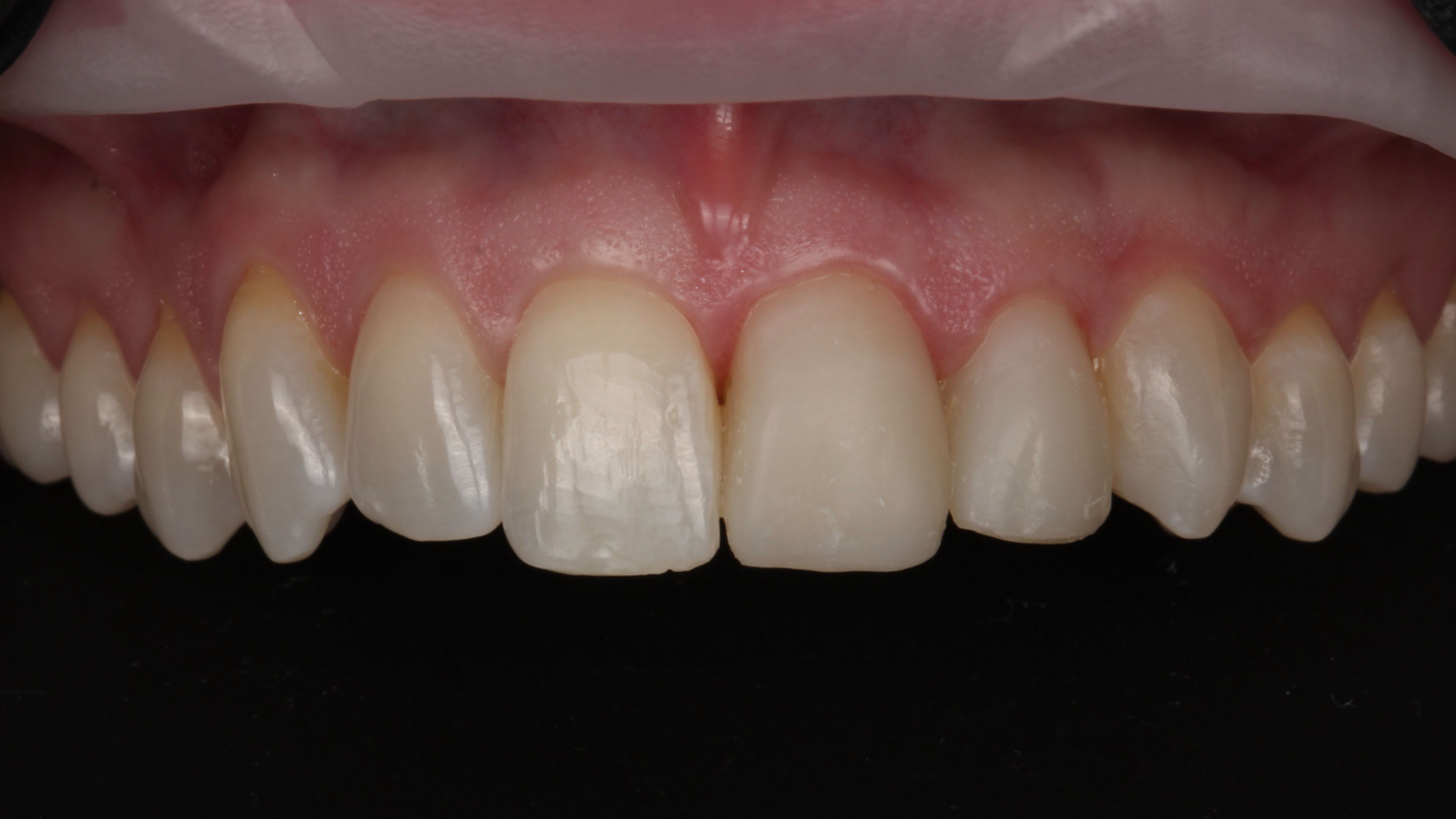
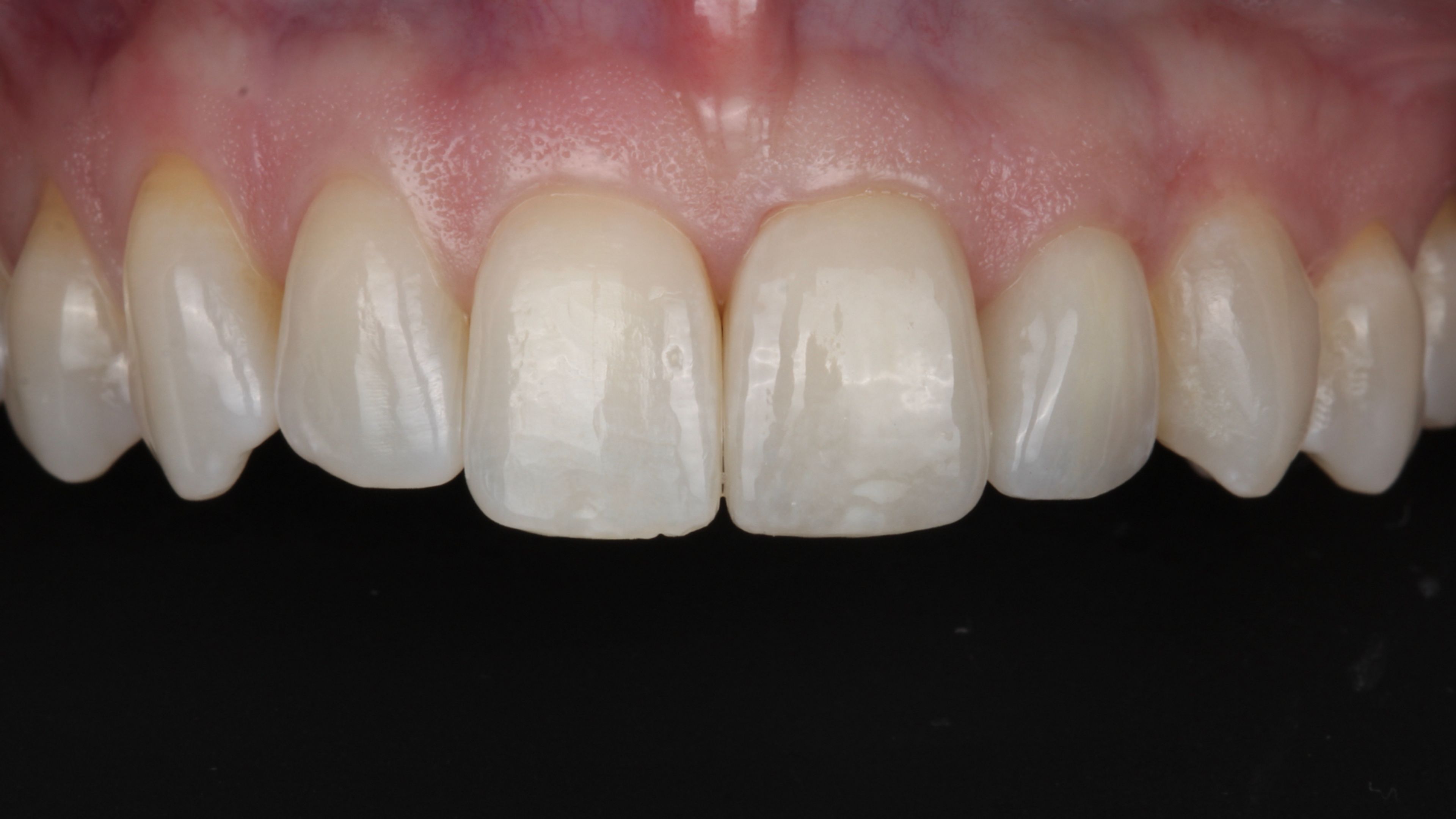
What it's like to be on the other side
Most patients describe the days after a redo as a relief more than anything else. The visual reminder of the work they didn't like is gone. The chronic gum irritation, when that was part of the picture, starts to settle within a few weeks. Bite issues that have been low-grade for months often resolve quickly once the new restorations are in occlusion.
Mild sensitivity in the first few days is normal, especially after larger cases. Most of it fades within a couple of weeks. The bite often takes a few visits to dial in perfectly — small adjustments are part of the process and not a sign anything is wrong.
Emotionally, the experience varies. Some patients arrive resigned, having lived with their dental work long enough that they no longer expect to feel good about it. Watching them see the new result for the first time is one of the more rewarding parts of doing this work.
The honest tradeoffs
A redo is a real investment. Worth knowing going in:
Cost. A redo is its own significant investment, separate from whatever was paid for the original work. Insurance rarely covers replacement of restorations that are technically functional, even when they aren't functioning well.
Time. The full process — consultation, design, removal, temporaries, fabrication, try-in, final — usually spans several weeks. Larger cases longer.
Tooth structure. Even with atraumatic laser removal, the teeth have already been prepared once for the original restoration. Atraumatic removal preserves what's there, but it can't restore what was removed by the original prep. The new restorations work with whatever foundation the original case left behind.
Emotional energy. Going through cosmetic dentistry a second time, sometimes with reasonable concern about whether this attempt will end better, is its own kind of investment. We take that seriously and pace the process so the patient is fully on board at each stage rather than rushed through it.
What to ask before you commit to a redo
If you're considering a redo, the consultation matters. The right questions reveal which clinics know how to do this well and which are simply willing to.
Diagnosis:
- Why did the original work fail? What specifically went wrong, and how does the new plan address it?
- Are you confident the new approach will produce a different outcome — and why?
Removal:
- How will you remove the existing restorations? What tools do you use?
- How do you protect the underlying tooth structure during removal? Are you using laser-assisted removal or conventional cutting?
- What does post-removal sensitivity typically look like with your technique?
The lab:
- Who fabricates the new restorations? Is the lab in-house or external?
- How do you communicate iterations between the clinical team and the lab team? How long does an adjustment take?
- Will the lab team be involved in the diagnosis of why the original failed, or only in fabricating the new work?
Process:
- What does the temporary phase look like? Will I have a real test-drive period?
- Will my feedback during temporaries be incorporated into the final design?
- Can I see photos of redo cases you've done — not first-time cases, but cases where you replaced someone else's work?
Honest assessment:
- Under what circumstances would you tell me to leave my current restorations alone? Is there a version of this consultation where the recommendation isn't to redo?
A clinician who can answer the last question well is a clinician you can trust to recommend a redo only when one is genuinely indicated.
The bottom line
Redoing dental work is a different craft from doing it the first time. The diagnostic question is harder — what failed, and why. The removal step matters in a way it never does on a virgin tooth. The lab partnership matters more, because the patient already knows what they don't want. The clinician needs experience seeing how cases fail, not just how they succeed, in order to design a redo that ends differently.
A meaningful share of the work we do is replacing work someone else started. We're glad to do it, the technology and team we've built around it makes the outcomes better than they otherwise would be, and we're matter-of-fact about saying when a redo isn't warranted.
If you've had cosmetic or restorative work that doesn't feel right — aesthetically, functionally, or in your gums — the next step is a conversation. We can look at what's there, talk through what's bothering you, and tell you honestly whether a redo is the right call.